Our Work to Promote Health Equity

Health equity is achieved when every person has the opportunity to attain their full health potential, and no one is disadvantaged from achieving this potential because of social position or other socially determined circumstances.1
Long-standing disparities in our healthcare system are well documented. B. Braun is responding by working in our communities to help people gain access to high-quality healthcare, developing technologies that address the individual characteristics and needs of each patient, partnering with leading healthcare organizations to gather data and advocate for improved standards of care, and raising the level of understanding about social determinants of health and inequities that have prevented many from achieving their full potential in life.

Examples of Health Disparities
- Racial and ethnic minority populations experience higher rates of poor health and disease in a range of health conditions, including diabetes, hypertension, obesity, asthma and heart disease, when compared to their White counterparts.3
- Black women are three times more likely to die from a pregnancy-related cause than White women.4
- Opioid overdose deaths are 45% higher in rural areas, yet urban patients have easier access to treatment facilities.5
- The historical underrepresentation of minorities and women in clinical trials has created gaps in understanding treatment effectiveness across populations.6




B. Braun’s Health Equity Strategy
We are working to make a difference in five key areas:

Workforce – We provide high-quality healthcare benefits for our employees, promote wellness programs and foster a diverse and inclusive culture across our company.
Community – We partner with local organizations to help raise awareness of health inequities and address access and social determinants of health in our communities.
Research – We work with leading healthcare and professional organizations to promote scientific research on health equity and access to healthcare.
Outcomes – We collaborate with health systems to support the use of technologies and programs to improve health outcomes and help ensure access to quality healthcare.
Advocacy – We advocate for policies to address healthcare disparities and raise standards of care to allow every person to attain their full health potential.
Addressing Disparities in Vascular Access
Peripheral vascular access is the most common invasive procedure performed in healthcare,7 but the experience of receiving an IV is not the same for all patients.
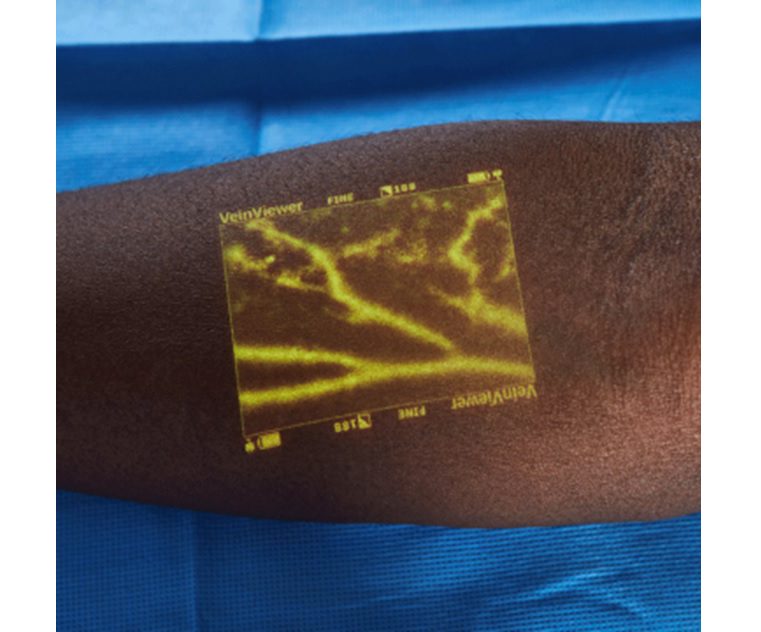
Photo Source: Christiemed.com
- In a study of over 100,000 emergency department (ED) patients, the rate of difficult intravenous access (DIVA) was 58% higher for Black patients compared to White patients (4.9% rate for Black; 3.1% rate for White).8
- This disparity exists despite the availability of vein visualization technologies and programs such as Peripheral Advantage®, which has been shown to improve peripheral vascular access outcomes.9
- B. Braun is working with leading healthcare organizations including the National Health Council and Association for Vascular Access to build awareness of this issue and promote more equitable vascular access treatment.
References:
1 Centers for Disease Control; https://www.cdc.gov/chronicdisease/healthequity/index.htm
2 US Department of Health and Human Services; https://health.gov/healthypeople/priority-areas/social-determinants-health
3 Centers for Disease Control and Prevention, Impact of Racism on our Nation’s Health; https://www.cdc.gov/minorityhealth/racism-disparities/impact-of-racism.html
4 Centers for Disease Control and Prevention, Working Together to Reduce Black Maternal Mortality, April 6, 2022; https://www.cdc.gov/healthequity/features/maternal-mortality/index.html
5 Association of American Medical Colleges, Health Disparities Affect Millions in Rural U.S. Communities, October 31, 2017; https://www.aamc.org/news-insights/health-disparities-affect-millions-rural-us-communities
6 National Institute on Minority Health and Disparities, Diversity and Inclusion in Clinical Trials; https://www.nimhd.nih.gov/resources/understanding-health-disparities/diversity-and-inclusion-in-clinical-trials.html
7 Tripathi S, Gladfelter T. Peripheral intravenous catheters in hospitalized patients: Practice, Dwell times, and factors impacting the dwell times: A single center retrospective study. J Vasc Access. 2021 Mar 30:11297298211000874. doi: 10.1177/11297298211000874. Epub ahead of print. PMID: 33784876.
8 Shokoohi H, Loesche MA, Duggan NM, Liteplo AS, Huang C, Al Saud AA, McEvoy D, Liu SW, Dutta S. Difficult intravenous access as an independent predictor of delayed care and prolonged length of stay in the emergency department. J Am Coll Emerg Physicians Open. 2020 Aug 19;1(6):1660-1668. doi: 10.1002/emp2.12222. PMID: 33392574; PMCID: PMC7771794. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7771794/
9 B. Braun Data on File: These are the results of FirstHealth of the Carolinas. Results and clinical experiences may vary by institution.
